A 64-year-old woman in New South Wales, Australia, unknowingly hosted a parasitic worm never before documented in humans. The case, recently detailed in medical reports, highlights the risk of zoonotic infections – diseases that jump from animals to people – and underscores how little we still understand about the natural world.
Initial Symptoms and Misdiagnosis
The patient first sought medical attention after experiencing prolonged abdominal pain, diarrhea, and a persistent dry cough accompanied by night sweats. Initial CT scans revealed inflammation in her lungs and lesions on her liver and spleen. Doctors misdiagnosed her with eosinophilic pneumonia, a rare lung condition, and prescribed steroids. While the medication provided temporary relief, her condition did not improve, and she returned weeks later with worsening symptoms.
Further testing ruled out common bacterial or fungal infections, as well as the presence of known parasitic flatworms. Despite traveling to regions where parasitic worms are prevalent, no antibodies or evidence of these parasites were found in her system. Doctors prescribed ivermectin, a treatment for parasitic worms, but the patient’s respiratory distress persisted.
The Unexpected Discovery
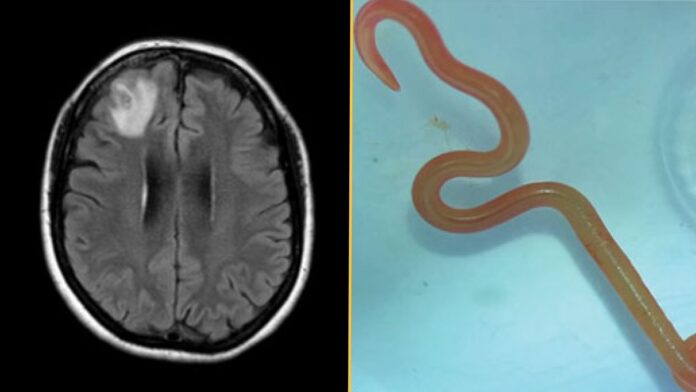
After nearly a year of unresolved symptoms, the woman began experiencing neurological changes: depression and forgetfulness. An MRI revealed a lesion on her brain’s frontal lobe. A subsequent biopsy uncovered the astonishing truth: a live, 3-inch-long parasitic worm embedded in her brain tissue. The worm was identified as a third-stage larva of Ophidascaris robertsi, a nematode typically found in carpet pythons native to Australia.
Treatment and Recovery
Doctors surgically removed the worm and treated the patient with a combination of ivermectin and albendazole, along with a course of dexamethasone to reduce inflammation. Six months after surgery, scans confirmed the lesions in her lungs and liver had disappeared, her white blood cell count normalized, and her neuropsychiatric symptoms improved.
Why This Matters
This case is unique because O. robertsi had never been documented to infect humans before. The parasite’s life cycle typically involves carpet pythons, where adult worms reproduce. The woman likely contracted the infection through contaminated wild greens she foraged near her lakeside home, ingesting eggs that hatched inside her body.
The longevity of the larval infection – comparable to those seen in laboratory rats – suggests that such undetected parasitic infections may be more common than previously assumed. The case highlights the growing threat of zoonotic diseases, driven by habitat encroachment and increasing human-animal interactions. It also underscores the need for broader surveillance of emerging parasitic threats in both wildlife and human populations.
This discovery reinforces the interconnectedness of ecosystems and the potential for novel pathogens to cross species barriers, demanding vigilance and continued research in public health.